AERB License for X-Ray Facilities in India: e-LORA Process, QA Requirements, Shielding Norms & Compliance Guide
Learn how to obtain an AERB license for X-ray facilities in India. Understand the e-LORA process, QA benchmarks, shielding requirements, TLD badges, RSO roles, and CDSCO compliance.
AERB & REGULATORY GUIDE
3/14/20265 min read


Navigating AERB Compliance: The Ultimate Guide to Licensing for X-Ray Facilities in India
The mission of the Atomic Energy Regulatory Board (AERB) is to ensure that the use of ionizing radiation and nuclear energy in India does not cause undue risk to the health of people and the environment. In the diagnostic imaging landscape, radiation safety is not merely a clinical preference but a strict legal mandate under the Atomic Energy (Radiation Protection) Rules, 2004, and the Atomic Energy Act, 1962. For healthcare providers, industrialists, and security professionals, obtaining an AERB license is the most critical step in establishing a compliant and safe radiation installation.
This comprehensive guide explores the "when," "why," and "how" of AERB licensing, drawing from official safety codes, training modules, and technical benchmarks to fulfill the search intent of professionals in the X-ray industry.
When is an AERB License Required?
The core regulatory principle is clear: no diagnostic X-ray equipment shall be operated for patient diagnosis until a valid Licence for Operation is obtained. This legal requirement applies to every stage of the equipment's life cycle, from manufacture and supply to commissioning and final decommissioning.
Mandatory Categories for Licensing: The requirement spans a vast range of "hot" product categories currently utilized in the medical and industrial sectors:
Medical Diagnostic Radiography: Fixed units, mobile X-ray units (wheeled), and portable units (intended to be carried, weighing under 12 kg).
Specialized Medical Systems: Computed Tomography (CT), Interventional Radiology (IR), C-Arm, Mammography, and Bone Mineral Densitometers (BMD).
Dental X-Ray Systems: Intra-oral Peri-apical (IOPA) including handheld units, Panoramic OPG, and Dental Cone Beam CT (CBCT).
Security and Research: X-ray Baggage Inspection Systems (XBIS), Portable X-ray Scanners (PXS), X-ray Diffractometers (XRD), and X-ray Fluorescence (XRF) devices.
The e-LORA Portal: The Gateway to Compliance
AERB has modernized the consenting process through the e-LORA (e-Licensing of Radiation Applications) portal. All regulatory transactions—from registering an institute to reporting a decommissioning—must be performed via this web-based system.
Step-by-Step Licensing Workflow:
Institute Registration: The facility must first register on the e-LORA portal with valid login credentials, including a registered email and mobile number.
Procurement Permission: Before buying equipment, the facility must apply for a Procurement Letter. This requires identifying a specific AERB Type Approved model and an authorized supplier.
Receipt and Installation: Upon equipment delivery, an authorized engineer must install the unit and generate an Installation Report.
Mandatory Quality Assurance (QA): A third-party agency authorized by the AERB must conduct a QA check to ensure the equipment meets technical safety benchmarks.
Final Application for Licence: The licensee uploads the Installation and QA reports to e-LORA. Approval for the Licence for Operation typically takes around 30 days.
Manpower and Staffing Requirements
A license cannot be granted unless the facility employs qualified professionals who understand radiation protection.
Qualified Operators: Facilities must have a radiologist, related medical practitioner, or a technologist who has passed from a recognized institution.
The Radiological Safety Officer (RSO): The facility (Employer) must designate an RSO, approved by the Competent Authority. For high-risk facilities like CT or IR, the RSO must be a radiologist or technologist with at least three years of working experience in the field.
Age and Health: No person under 18 years of age can be employed as a radiation worker.
Radiation Protection and Safety Tools
AERB licensing is contingent upon the availability of proper shielding and monitoring tools.
TLD Badges (Personnel Monitoring): Every radiation worker is mandated to wear a Thermoluminescent Dosimeter (TLD) badge to monitor their effective dose. For accuracy, the badge must be worn below the lead apron at the chest level.
Personal Protective Equipment (PPE): Operators must have access to lead aprons with a minimum lead equivalence of 0.25 mm. For interventional procedures, additional tools like thyroid shields, protective goggles, and ceiling-suspended screens (0.5 mm lead eqv) are required.
Mobile Protective Barriers (MPB): For rooms where the operator cannot stand in a separate control booth, a mobile barrier with a viewing window (minimum 1.5 mm lead equivalence) is mandatory.
Room Layout and Shielding Design
The physical environment of the X-ray installation is a primary factor in public and occupational safety.
Structural Shielding: Walls and doors of the X-ray room must provide adequate attenuation. For example, doors must have a lead lining of 1.7 mm.
Layout Safety: The chest stand should be positioned so that stray radiation does not reach the control console or entrance door. In CT and IR facilities, the control console must be in an adjoining room with a lead glass viewing window and oral communication facilities.
Warning Systems: A permanent radiation warning symbol and instructions for pregnant women must be posted at the entrance door.
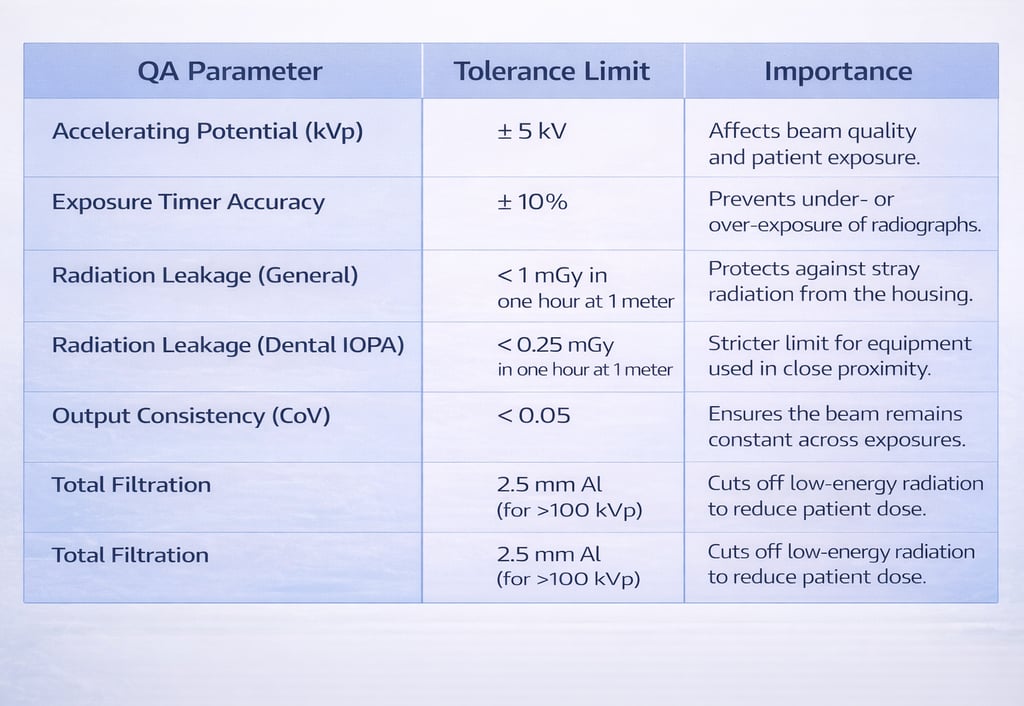
Quality Assurance (QA) Benchmarks and Tolerances
QA is a systematic action necessary to provide confidence that equipment performs satisfactorily in compliance with safety standards. Licensing requires an initial QA and subsequent testing once every two years or after major repairs.
Roles and Responsibilities: The Compliance Chain
Ensuring a safe radiation installation is a collective responsibility divided among four key roles:
The Employer:
Acts as the custodian of the equipment and holds ultimate responsibility for safety.
Ensures that only AERB Type Approved equipment is procured.
Designates the RSO and ensures no person under 18 is employed for radiation work.
The Licensee:
Establishes written procedures for controlling exposures.
Ensures periodic training for workers and arranges for the mandatory biennial QA tests.
Customizes exposure protocols, particularly for pediatric patients, to optimize dose.
The Radiological Safety Officer (RSO):
Advises the employer on safety aspects and ensures compliance with AERB rules.
Maintains records of QA and radiation surveys.
Verifies the performance of protective devices like lead aprons.
The Radiation Worker (Operator):
Undergoes training on safe operation and dose reduction.
Follows the ALARA (As Low As Reasonably Achievable) principle.
Uses TLD badges and protective gear religiously during operation.
CDSCO Integration and Legal Penalties
Beyond the AERB, X-ray machines in India are classified as Class C (Moderate to High Risk) medical devices. Since January 1, 2021, registration with the CDSCO (Central Drugs Standard Control Organization) is mandatory for import or manufacture. This regulation prevents the proliferation of inferior quality products that could lead to misdiagnosis.
Offences and Penalties: Non-compliance is a serious matter. Contravening any terms of the license or AERB rules is punishable under the Atomic Energy Act, 1962. Penalties include:
Suspension or cancellation of the license.
Financial fines.
Imprisonment, depending on the severity of the offence.
Conclusion
AERB licensing is the cornerstone of Expertise, Authoritativeness, and Trustworthiness (E-E-A-T) for any modern diagnostic or industrial facility. By strictly following the e-LORA process, maintaining bi-annual Quality Assurance, and adhering to ALARA-based operational safety, facilities can leverage "hot" X-ray products to their full potential while ensuring the absolute safety of patients, staff, and the general public. Compliance is not just a regulatory obligation; it is a commitment to the highest standards of diagnostic excellence and human safety.
About XRAYNNEWS.NET
XRAYNEWS.NET provides updates on medical and industrial X-ray technologies, radiography insights, regulatory awareness, and imaging industry developments.
Regulatory Resources
© 2025. All rights reserved.
Video Resources
Popular Topics
Quick Links
Stay Updated with X-Ray Industry News
Subscribe to receive updates on X-ray technology developments, radiography insights, and industry news.
