High-Frequency X-Ray Generators: Benefits, Safety & Why Modern Systems Are Replacing Conventional Technology
Explore how high-frequency X-ray generators improve image quality, reduce radiation dose, and meet AERB compliance, making them the modern standard in radiology.
INDUSTRY INSIGHTS & TECHNOLOGY
3/19/20264 min read
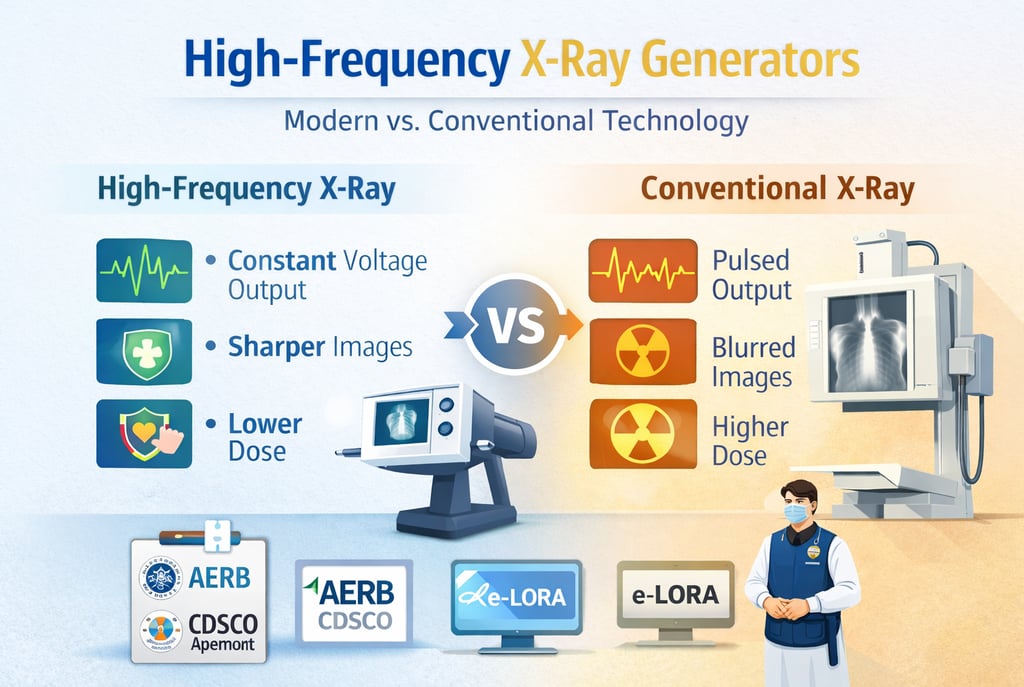
High-Frequency X-Ray Generators: Why Modern Systems Are Replacing Conventional Technology
The radiological landscape in India and globally is witnessing a decisive transition from conventional low-frequency systems to high-frequency (HF) X-ray generators. This shift is driven by the fundamental objective of the Atomic Energy Regulatory Board (AERB): to ensure that the medical use of ionizing radiation provides maximum diagnostic benefit with minimum risk to patients, staff, and the environment. Modern HF technology, particularly those utilizing constant potential output, has become the authoritative standard for clinical excellence. By optimizing the X-ray beam and reducing patient dose, these systems fulfill the critical regulatory mandate of ALARA (As Low As Reasonably Achievable).
1. The Technological Advantage: Waveform Efficiency and Constant Potential
The primary distinction between conventional and high-frequency generators lies in the efficiency of the electrical waveform used to produce X-rays. Conventional systems often utilize a pulsating waveform where the voltage fluctuated, leading to the production of low-energy "soft" X-rays that increase patient dose without contributing to the diagnostic image.
Constant Potential Generation: Modern HF generators convert standard low-frequency power into high-frequency pulses before rectification and smoothing, resulting in a constant potential. This ensures the X-ray tube operates at the peak voltage (kVp) for the entire duration of the exposure.
Beam Filtration Standards: AERB mandates that equipment operating at constant potential must have a minimum total filtration of 2.5 mm Al equivalent. This filtration effectively cuts off unnecessary low-energy radiation, thereby optimizing radiation quality.
Technical Specifications: A comparison of modern HF handheld units (like the Nomad Pro) and conventional wall-mounted sources shows that HF units can achieve superior results at lower power settings—typically 60 kVp and 2.5 mA compared to 70 kVp and 8 mA for conventional units.
2. Enhancing Image Quality: The Role of Focal Spot Size and Resolution
High-frequency technology allows for more precise control over the X-ray source, which directly impacts the clarity of the diagnostic information obtained.
Smaller Focal Spot Size: A critical technical benchmark for modern HF units is the focal spot size, which is the area of the anode where X-rays are produced. Modern handheld HF units often utilize a 0.4 mm focal spot, whereas conventional wall-mounted units typically feature a larger 0.7 mm spot.
Line Pair (LP) Resolution: Because of the optimized focal spot, mean LP resolution—a measure of the ability to resolve fine detail—is significantly higher in modern HF systems. Research indicates mean LP resolution values of 6.05–6.55 lp/mm for HF handheld devices compared to 5.58–6.31 lp/mm for traditional wall-mounted sources.
Reduced Image Distortion: Proper central beam alignment (required to be within < 1.5°) is more easily maintained in modern, lightweight HF units, preventing image distortion and the loss of minute details that can occur with poorly aligned conventional systems.
3. Dosimetry and Safety: Achieving the ALARA Principle
One of the most compelling reasons for the replacement of conventional technology is the substantial reduction in radiation dose afforded by high-frequency systems.
Patient Dose Reduction: Clinical simulations of a Full Mouth Examination (FMX) demonstrate that the mean patient dose for HF handheld units is 36 µSv, significantly lower than the 98 µSv recorded for conventional wall-mounted sources. This represents a total effective dose reduction of approximately 12%.
Optimization of Exposure Factors: This dose reduction is attributed to the optimization of exposure factors (kVp, mA, and time) inherent in HF technology. HF units allow for shorter, more precise clinical exposure times (as low as 0.16s for anterior projections).
Operator Safety: Mean operator exposures for properly used modern systems are indistinguishable from ambient background levels (<2 µGy/study). Furthermore, modern portable units feature integrated internal and external shielding to protect the operator from scatter radiation.
4. Regulatory Compliance and the e-LORA Framework
In India, the transition to high-frequency systems is supported by a rigorous regulatory framework involving the AERB and the Central Drugs Standard Control Organization (CDSCO).
Class C Medical Device Classification: Since January 1, 2021, all X-ray machines have been classified as Class C (Moderate to High Risk) medical devices, necessitating mandatory CDSCO registration to prevent the use of inferior-quality products.
e-LORA Portal Registration: Facilities must manage the entire equipment lifecycle—from Procurement Permission to Licence for Operation—through the e-LORA (e-Licensing of Radiation Applications) digital portal.
Mandatory Quality Assurance (QA): The end-user is responsible for ensuring that periodic QA is carried out by authorized agencies once every two years. Key QA tolerances for modern systems include:
kVp Accuracy: Within ± 5 kV of the set value.
Timer Accuracy: Error not exceeding ± 10%.
Output Consistency (CoV): Less than 0.05.
5. Operational Flexibility: The Rise of Ultra-Portable Systems
The miniaturization enabled by high-frequency technology has led to the development of ultra-portable (UP) and handheld systems, which are transforming community-based diagnostics.
Field Utility: UP systems weigh not more than 12 kg and can be carried by one or two persons, making them ideal for Tuberculosis (TB) screening in areas without stable power supplies.
AI and CAD Integration: Modern digital HF systems are often paired with Artificial Intelligence (AI) and Computer-Aided Detection (CAD) software, which provides automated, standardized image interpretation—a vital tool in regions where expert human readers are scarce.
Remote Operation: For security and open-field medical scanning, modern systems allow for remote operation from a distance of at least 30 meters.
6. Institutional Roles and Safety Infrastructure
To maintain the high standards required for HF systems, facilities must establish a robust safety culture led by qualified personnel.
The Radiological Safety Officer (RSO): Every facility must designate an AERB-approved RSO responsible for radiation protection functions. For high-risk installations like CT or Interventional Radiology, the RSO must have at least three years of experience in the field.
Personnel Monitoring: All radiation workers are mandated to use TLD (Thermoluminescent Dosimeter) badges to monitor their cumulative annual dose, which must not exceed 20 mSv averaged over five years.
Protective Equipment: Despite the efficiency of HF generators, operators must always use mandatory protective gear, including lead aprons (minimum 0.25 mm lead equivalence) and mobile protective barriers (minimum 1.5 mm lead equivalence).
Conclusion: Why High-Frequency is the New Gold Standard
The replacement of conventional technology with high-frequency X-ray generators is a strategic move toward Expertise, Authoritativeness, and Trustworthiness (E-E-A-T) in clinical diagnostics. By providing a constant potential beam, HF systems deliver superior Line Pair resolution and significantly reduce patient and operator doses, adhering to the highest safety standards of the AERB and CDSCO.
For modern medical facilities, the decision to adopt HF technology is not merely a hardware upgrade; it is a commitment to diagnostic excellence and human safety. Through religious adherence to biennial Quality Assurance, meticulous e-LORA licensing, and the application of the Time-Distance-Shielding (TDS) principle, these systems ensure that diagnostic information is obtained at the lowest possible radiation risk. In the era of digital transformation and AI integration, high-frequency generation is the foundational pillar of modern radiology in India.
About XRAYNEWS.NET
XRAYNEWS.NET provides updates on medical and industrial X-ray technologies, radiography insights, regulatory awareness, and imaging industry developments.
Regulatory Resources
© 2025. All rights reserved.
Video Resources
Popular Topics
Quick Links
Stay Updated with X-Ray Industry News
Subscribe to receive updates on X-ray technology developments, radiography insights, and industry news.
